This article makes reference to certain companies and their products and any opinions expressed should not be taken to be the views of Dystonia Europe or its members. The articles are written by respected authors and are provided for the information of Dystonia Europe News readers.
The Medtronic BrainSenseTM Expert Meeting was originally planned as a face-to-face event in Barcelona. Due to COVID-19 limitations, the meeting was held virtually on May 11-12 2020, with an international faculty and chaired by Prof. Dr. Andrea Kühn, Head of Movement Disorders and Neuromodulation Section at Charité University Hospital of Berlin, and Priv.-Doz. Dr. med. Jan-Hinnerk Mehrkens, Head of Functional Neurosurgery of the University of Munich (LMU), Campus Grosshadern. Around 1,400 registered attendees followed the experts’ discussion about the latest clinical evidence on sensing in Deep Brain Stimulation (DBS) and the potential role that the recently launched Percept PC neurostimulator with BrainSense technology will play in better understanding DBS and applying adaptive DBS (aDBS) in future.

Prof. Dr. Andrea Kühn, Head of Movement Disorders and Neuromodulation Section at Charité University Hospital of Berlin

Neuromodulation Section at Charité University Hospital of Berlin, and Priv.-Doz. Dr. med. Jan-Hinnerk Mehrkens, Head of Functional Neurosurgery of the University of Munich (LMU), Campus Grosshadern
The Medtronic BrainSenseTM Expert Meeting was originally planned as a face-to-face event in Barcelona. Due to COVID-19 limitations, the meeting was held virtually on May 11-12 2020, with an international faculty and chaired by Prof. Dr. Andrea Kühn, Head of Movement Disorders and Neuromodulation Section at Charité University Hospital of Berlin, and Priv.-Doz. Dr. med. Jan-Hinnerk Mehrkens, Head of Functional Neurosurgery of the University of Munich (LMU), Campus Grosshadern. Around 1,400 registered attendees followed the experts’ discussion about the latest clinical evidence on sensing in Deep Brain Stimulation (DBS) and the potential role that the recently launched Percept PC neurostimu-lator with BrainSense tech-nology will play in better understanding DBS and applying adaptive DBS (aDBS) in future.
Today, DBS is a well-established therapy option to alleviate symptoms in patients with movement disorders and with inadequate or adverse response to medication. To date, electrophysiological recordings can be performed during implantation of the DBS device in order to position electrodes and therapy programming. After implantation, the window for discovery of deep brain signals is closed until the next stimulator replacement. As consequence, most of today’s evidence was obtained through brain recording by a complex experimental setup of externalized DBS electrodes without the possibility to collect long-term data. In 2013, Medtronic made an experimental sensing-enabled ActivaTM PC+S neurostimulator available to study centers worldwide that allowed LFP recordings by the implanted pulse generator (IPG). These intraoperative and postoperative studies in DBS patients have significantly contributed to today’s understanding of the pathological neural activity related to movement disorders. And even more, they inspired a new paradigm called adaptive DBS or closed-loop adaptive DBS (aDBS) leading away from the chronic DBS stimulation towards an intermittent and patient-specific stimulation in future.
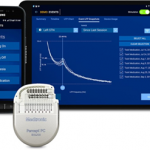
Percept PC neurostimulator:First DBS device with chronical brain sensing The launch of Percept PC neurostimulator in January 2020 is a crucial step on the way to an a DBS. It is the first DBS device with commercial brain sensing technology recording signals from the brain to understand the patient state inside and outside of the clinic.
The dual channel recharge-free Percept PC neurostimulator is approved for Parkinson’s disease, essential tremor, dystonia, epilepsy and obsessive-compulsive disorder.
Steve Goetz, Engineering Director, Technology, Strategy and Business Development at Medtronic PLC (USA) presented the details of this technological innovation. For decades Medtronic is committed to research and development in the field of DBS. As a result of this intensive development effort, the new Percept PC neurostimulator features a completely redesigned and ergonomic platform: First, it is a 3 Tesla MRI compatible system in addition to the 1.5 Tesla MRI safety Medtronic DBS devices already had previously. The 3 Tesla feature allows many more diagnostic and clinical scans as well as research activities. Moreover, the Percept PC neurostimulator is 20% smaller and thinner and it has a 15% longer service life for the average patient due to advances in battery technology.
The innovation of Percept neurostimulator goes far beyond. It is the first device with BrainSense technology delivering a commercial sensing capability to record brain signals (local field potential, LFP) chronically using the implanted DBS leads. These signals can be recorded simultaneously while delivering therapeutic stimulation, inside and outside the clinic. Based on these data, the physician may adjust DBS stimulation settings, thereby personalizing therapy towards best possible treatment outcomes.
“The BrainSense technology has the potential to be disruptive”, states Goetz. “It gives us unprecedented insights into the patients experience and the disease state. This window into the patient hasn’t existed before.” The Percept PC Neurostimulator uses embedded software for processing and analysis of brain signals in real time. These signals are stored on the device and can be viewed using the intuitive clinician programmer. They can also be exported in JSON, a machine-readable format, for offline data processing.
Several analysis tools are available for sensing. Outside the clinic, BrainSense Timeline can analyze the brain state during a long period of time. The tool captures previous 60 days of 24/7 real world data. “This is a powerful tool”, explains Goetz. “You can identify changes of a signal over time, assess changes due to medication or check the impact of daily activities like sleep, wake and meals.” In addition, the patient him/herself can mark events of interest with BrainSense Events on his/her patient programmer. This tool helps to understand signals at a certain point of time. Events can be compared, and trends can be identified.
Inside the clinic, the BrainSense technology offers two more features: The BrainSense Survey allows the physician to understand the neuronal landscape. It shows which LFP signals are available across electrodes, type and location of signals. If there is a signal of interest that correlates with aspects of the patient state like rigid or kinetic symptoms, it can be clinically explored with BrainSense streaming. “This important element allows you to adjust stimulation and to understand how DBS stimulation is impacting the signal in the presence of stimulation”, explains Goetz, this is real time access to the brain state.
With these sensing tools, the physician can capture signals in the brain that correlate with the patient state, understand how stimulation impacts these signals over time and adapt the stimulation to patient specific brain state avoiding side-effects and/or saving battery energy. Besides the individual treatment of patients, Steve Goetz also points out the potential for aDBS: “Extending this idea of unprecedented insight, we really do believe that the idea of chronical brain monitoring is foundational. We can understand what is happening over long periods of time to signals of interest”, he says.
Clinical evidence of biomarkers in Parkinson’s Disease and Dystonia
Andrea Kühn showed which symptom-specific patterns of neuronal activity could be used as a feedback signal for adaptive stimulation based on the extensive research work in Berlin, but also by other international research groups. This study work was initially carried out using externalized leads and later with the Activa PC+S device which allowed for the first time a chronic recording from PD and Dystonia patients. In order to investigate the feasibility of subthalamic recordings via a chronical IPG, the Charité team obtained subthalamic LFPs from eight PD patients before and during DBS with Activa PC+S, ON and OFF stimulation conditions were also analyzed. The results showed that oscillatory beta band synchronization and its modulation by DBS is recordable with the system and may serve as a biomarker for subthalamic closed-loop stimulation in PD patients. Even more, the group could show that beta activity is a stable long-term biomarker in PD and that beta activity correlates with improvement of motor impairment.
“In dystonia we know a little bit less”, said Kühn. “But even in dystonia we have a potential biomarker which needs to be explored further.” Kühn showed results from dystonia patients that underwent DBS at Charité Berlin. Irrespective of the type – generalized, segmental or cervical dystonia – similar patterns of low frequency activity could be found. In addition, symptom severity of motor deficits correlates with pallidal theta activity (4-12 Hz) while beta activity did not correlate with the motor symptoms.
A further study1 with the Activa PC+S device could show that low‐frequency activity is associated with dystonic motor sign severity, even months after chronic DBS. LFPs were recorded in 9 dystonia patients at 5 timepoints during an OFF‐stimulation period of 5 to 7 hours in parallel with clinical assessment using Burke‐Fahn‐Marsden Dystonia Rating Scale. The results showed a significant association of increase in the Burke‐Fahn‐Marsden Dystonia Rating Scale scores with recurrence of low‐frequency activity across timepoints after DBS was switched OFF. This underlines the potential utility of low frequency activity as a biomarker in dystonia for aDBS.
Percept PC neurostimulator: First experiences with the new device
Six centers across Europe shared their first experiences with the Percept PC neurostimulator during the Medtronic BrainSense Expert Meeting. The very first implantation of the Percept device was realized Jan-uary 14th at Charité, Berlin. Andrea Kühn shared the first recordings after the pulse generator exchange in a female dystonia patient who had already benefitted from a pallidal stimulation for a few years. With these recordings, Kühn could confirm again the research work of her team regarding dystonia-specific bio-markers at low frequency. With the BrainSense Survey mode the team could record the neuronal landscape in a bipolar mode from different contacts. “In comparison to the Activa PC+S device, the data quality is much better now with the new device”, Kühn said. It even allowed the analysis of the interhemispheric coherence with the low frequency peaks.
With the second patient, a young man with generalized dystonia, the Berlin team did the recording with the BrainSense Streaming mode allowing analysis in the time frequency domain and titrating the stimulation therapy. Finally, Kühn shared the first pilot data using the BrainSense Timeline mode. Outside the clinic, the low frequency activity of the patient was recorded over 60 days at different time points. The findings are activity drops overnight and increased activity over the day. Over the complete time period of 60 days one could hypothesize that the low frequency activity is slightly diminished over time. “There could be some long-term effect, but of course we will need much more data”, said Kühn.
“We have beta activity and theta activity as a start, but we will learn much more with the chronic sensing device now, and we will hopefully be able to use this for aDBS in our patients”, Kühn closed her lecture.
The very first implant of Percept PC neuromodulator in Parkinson’s disease in the STN took place at the University Hospital in Munich January, 15th (DBS electrodes) and January 17th (IPG). Jan-Hinnerk Mehrkens presented the case of a 56-year old male PD patient with a disease duration of about 12 years. The patient developed severe on and off fluctuations in 2018 which was the indication for a DBS implantation (UPDRS III baseline score: On med 16, Off med 38). During surgery (bilateral STN, patient awake, MER incl LFPs), rigidity symptoms vanished completely on stimulation. First data recordings could be captured one hour postop on the ICU: “We saw nice readings in the left and right STN, great peaks in the beta range on both sides”, reported Mehrkens. Also, the first programming 4 days postop, showed instant effects on symptoms.
Being a neurosurgeon, Mehrkens mentioned the new Percept device to be well-shaped, allowing a robust data acquisition. He also judged the handling of BrainSense modes to be easy for physicians and patients.
Outlook: The promise of sensing
Mark Richardson, MD, PhD, Director Functional Neurosurgery at Massachusetts General Hospital and Member of the Neurosurgical Faculty at Harvard Medical School, USA, showed the enormous research effort that is being put into study activities on DBS globally. The Medtronic Engineering Group has played a large part in this, Richardson said, performing groundbreaking work that shows the future potential of DBS.
Although the main topic of discussion in the context of DBS is Parkinson’s disease, there is potential for all different types of brain disorders because they can be understood as network disorders. “There is an immense potential for how we use the sensing information”, notes Richardson. The condition for this is the identification of reliable electrographic biomarkers of response to closed loop stimulation.
Following Richardson, there are still some open questions, which can now be partially clarified with the new clinical sensing experience. These questions include hardware issues such as the use of the same electrode for stimulation and sensing, as well as the idea of placing subcortical or cortical sensors outside the DBS target area. Another important question is how to involve the patient. “This question can be transformative”, said Richardson. “What obligations do we have to share this information with patients? How can patients use this information? Can these tools be used to help engage them overall in improving their quality of life?”
Finally, Richardson outlined the promise of sensing, showing the potential evolution of this technology in future. Currently, sensing-enabled DBS is going to provide a lot of useful data. However, the physician will need to manually adjust the device and the medication. In a not too far future, stated Richardson, a DBS device will provide relatively simple automated DBS adjustments. The vision ahead would be an intelligent adapted DBS using Artificial Intelligence. Such a device would have the ability to teach itself when the next maneuver should be done using brain information.
Peter Brown, Professor of Experimental Neurology at the University of Oxford and Consultant Neurologist at Oxford’s John Radcliffe Hospital, Oxford (UK), added why aDBS could be useful. The state of the art in Parkinson’s disease today is continuous stimulation at constant frequency which is clearly beneficial. But it also has side-effects like gait and speech impairment, brittle dyskinesias or mood changes. The idea of aDBS is to modulate delivery of DBS according to feedback indi-cative of motor impairment. While the first motivation is the reduction of side effects this concept also aims for a better symptom control and saving of energy.
A crucial question, according to Brown, is what can be used as feedback for aDBS. On the one hand, brain signals must be robust enough, and they have to be registerable with a sufficient amplitude. On the other hand, they also need to correlate with aspects of movement impairment like finely tuned gamma activity does with dyskinesia and beta activity does with bradykinesia-rigidity.
A further question is how feedback is used. “How feedback modulates DBS is determined by something called the `control policy´”, explained Brown. The simplest control policy is threshold control, as used in air con-ditioning. When temperature rises above a certain threshold, this is detected by a thermostat and air conditioning reduces temperature. “The choice of control policy for aDBS in PD will depend on our understanding of the nature of beta activity, or other biomarker activity, and on technical constraints. We are in a great need of a chronic trial of aDBS to show if it is chronically effective”, stated Brown.
The Percept PC neurostimulator now offers a way to take this next step on the road to aDBS. James Eubanks, Director of Clinical Research for Brain Modulation at Medtronic plc (USA) announced the upcoming ADAPT-PD clinical trial for Parkinson’s disease, which will start after commercial release of the Percept device in the US. Together with study sites in Europe, US and Canada, this pre-market IDE approval study will assess safety, tolerability and efficacy of different aDBS programs in comparison to conventional DBS baseline. The aDBS features for this trial are already enabled in Percept PC neurostimulator and will be unlocked for the study centers to deliver evidence.
- Scheller U, Lofredi R, van Wijk BCM, et al. Pallidal low-frequency activity in dystonia after cessation of long-term deep brain stimulation. Mov Disord. 2019;34(11):1734-1739. doi:10.1002/mds.27838